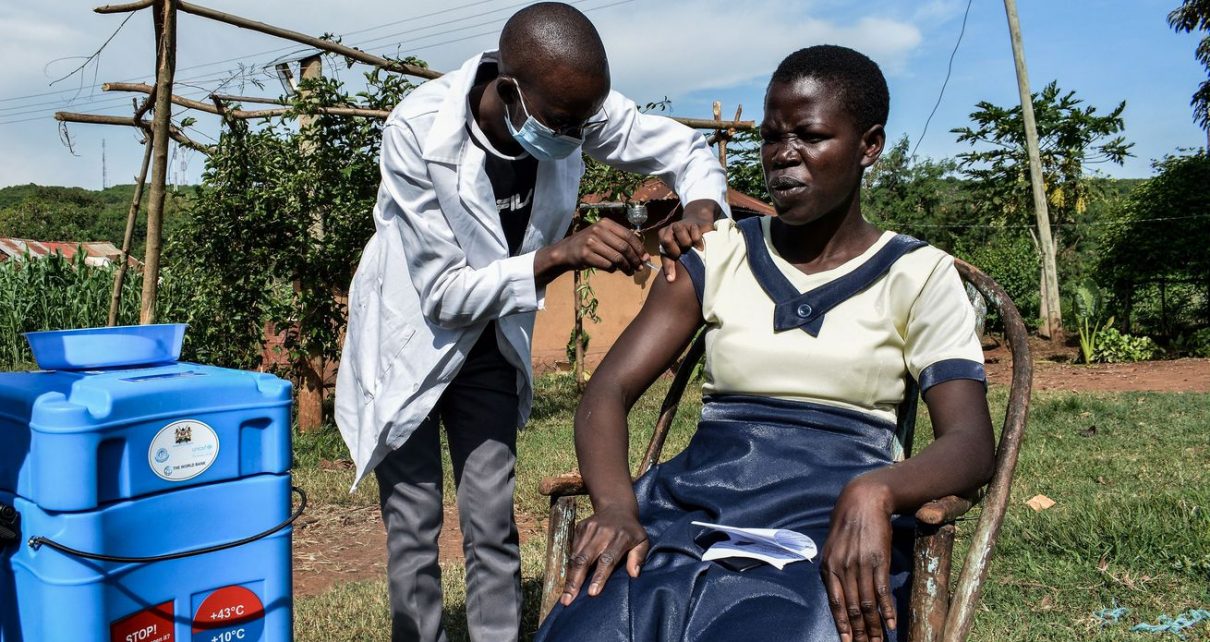
Covax wanted to send 2 billion doses worldwide this year. It’s 3.4 percent of the way there.
Early on in the pandemic, global health experts envisioned a nightmare scenario: Covid-19 vaccines are created, but they go almost exclusively to rich countries that can afford to buy them. People in poorer countries are left to get sick and die.
To prevent this, the experts set up an international initiative called Covax, designed to make sure every country in the world gets access to vaccines regardless of its ability to pay. In the fall of 2020, Covax set a clear goal: Buy 2 billion doses and make them available to nations in need before the end of 2021.
But we’re now nearly five months into the year, and Covax has delivered just over 68 million doses. In other words, it’s only 3.4 percent of the way to its goal.
The nightmare has become reality. Around 1.5 billion vaccine doses have been administered around the world — yet only 0.3 percent have gone to low-income countries. And in places like India and Brazil, thousands of unvaccinated people are dying every day of Covid-19, even as many Americans revel in their vaccinated status.
“People keep asking me, ‘What keeps you awake at night? The variants?’ Christ, no! It’s human behavior — the unwillingness to share!” said Bruce Aylward, a senior adviser at the World Health Organization (WHO) who works on Covax. “How do other people sleep at night? They should be so energized to fix this!”
If the epidemiologist and his colleagues at Covax have not managed to avert global vaccine inequity, it’s not for lack of trying. They’ve gotten life-saving doses to 124 countries from Argentina to Zambia, and they’ve pushed wealthy countries to help them do more.
“Covax has been an essential tool. I think that’s pretty indisputable,” said Kate Dodson, the vice president for global health at the UN Foundation. But, she added, “They’re struggling right now.”
So what explains Covax’s struggles? What are the biggest obstacles getting in the way?
The experts I talked to identified three main problems: money, vaccine supply, and global willingness to share have all been too constrained. But, the experts emphasized, these are solvable problems. And there are things everyday individuals can do to help.
/cdn.vox-cdn.com/uploads/chorus_asset/file/22524891/bruce_aylward_GettyImages_1203152203.jpg) AFP via Getty Images
AFP via Getty Images“The money was insufficient, and the money was late”
The WHO is one of three groups leading Covax. The other two are Gavi, a public-private partnership that spearheads immunization efforts in developing countries, and the Coalition for Epidemic Preparedness Innovations, an international collaboration (formed as a Gates Foundation initiative after the West African Ebola epidemic) to make vaccines available quickly when outbreaks happen.
All three groups have collaborated to make Covax into a unique, not-for-profit, financing mechanism. It’s designed to work kind of like a mutual fund, but for vaccines. The idea was that high-income countries would pool their money together to fund research and development for a diversified portfolio of vaccine candidates. That investment would up the chances that they’d land on an effective vaccine, and it would also serve to fund free vaccine doses for 92 lower-income countries that couldn’t afford to pay.
It sounded like a win-win. But for it to work as planned, enough rich countries had to buy into Covax and commit to getting their doses through the fund.
Instead, many governments made separate bilateral deals with companies like Pfizer and Moderna, locking up in contracts the vast majority of doses slated to be produced in 2021. That robbed Covax — which didn’t have much money on hand in the early stage of the pandemic — of the opportunity to buy vaccines for less wealthy countries.
“The main issue is that the money was insufficient, and the money was late,” said Amanda Glassman, director of global health policy at the Center for Global Development, a nonprofit think tank based in London and Washington, DC. “If they’d had all the money in March 2020, we’d be in a different space in terms of the delivery. There was more wiggle room in March through July of last year to reserve doses if they’d had the money in place.”
Covax was stymied in its ability to buy. And even now, it still doesn’t have the funding to buy enough vaccine doses to cover 20 percent of the population in each low-income country — the health care workers and most vulnerable groups — by the end of 2021. To achieve that, it needs to raise another $2.6 billion.
Aylward was clear that that remains Covax’s foremost obstacle. “The first thing we need is money,” he said.
You might wonder how much good it would do for Covax to have more cash on hand right now. With so many doses already locked up in contracts, would extra money get shots into arms any faster?
The experts I spoke to acknowledged that it wouldn’t enable people in low-income countries to get shots tomorrow, but it would certainly bump up the timeline. For some populations, it could mean being immunized in the third quarter of 2021 rather than the fourth; for others, it could mean the difference between early- and mid-2022.
It’s crucial for Covax to get more funding now because it will need cash in hand to buy more of the vaccines that are starting to coming online, such as Novavax (an American-made vaccine) and Sinopharm (a vaccine created in China and recently approved for emergency use by the WHO). By June, Covax needs at least $1.6 billion above currently secured funding in order to lock in doses for 2021 and early 2022, a Gavi spokesperson said. Otherwise, the doses may get snatched up by wealthy countries just like they did in 2020.
“Supply is incredibly tight”
The second huge challenge facing Covax is the simple fact that vaccines and the raw materials needed to make them are still in short supply.
That’s partly because rich countries bought up a lot of the early vaccine supply, as noted above. But it’s also because the pandemic itself sometimes makes it hard to stick to a production schedule.
The main supplier to Covax is the Serum Institute of India, which produces the AstraZeneca vaccine. But with Covid-19 currently raging in India, the supply has been necessarily turned to domestic use. Export restrictions mean that Covax is receiving much less vaccine than expected and has had to delay its shipments to countries.
As Dodson said, “Supply is incredibly tight for Covax.”
It’s a good illustration of why we need a global plan to increase the scale and security of vaccine production.
“We need a way to — faster than it’s ever been done before, globally, in concert — work to dramatically increase the number of vaccine doses that are going to be available in 2021 and early 2022,” said Ruth Faden, a founder of the Johns Hopkins Berman Institute of Bioethics, who co-drafted the WHO’s Values Framework for vaccine allocation. “Really what you would want to see is an Operation Warp Speed at the global level.”
That won’t be an easy operation to pull off, because it’s not just a matter of building more plants with more production capacity in more countries. It’ll require coordination on a number of underlying factors — transferring technological know-how and personnel to countries in need, sending raw materials to prevent manufacturing bottlenecks, and loosening intellectual property rights. (The Biden administration’s decision to support patent waivers for Covid-19 vaccines will hopefully help with the latter.)
Aylward emphasized that it’s not enough to just scale up production — a good part of that production needs to be earmarked for Covax. As companies learn how to optimize their capacity, he wants them to give Covax the right of first refusal on any vaccine they produce in excess of their original targets.
“We need people to share”
Last but not least, Covax needs wealthy countries to share.
That can mean sharing doses that have already been delivered. The US, for instance, currently has about 73 million doses sitting in its stockpile. But ideally, wealthy countries should donate doses even before they arrive on their shores.
“We don’t want them to receive doses and then say ‘You know what, we decided we don’t want this, we’ll give this to you,’” Aylward said. Transferring doses after they’ve been delivered can be tricky because of the need to guarantee that “chain of custody” is intact — that cold storage requirements, for example, were at no point interrupted. “We need people to share their space in the queue.”
In other words, when new vaccine doses come online, rich countries should not take up all the space at the front of the line to receive them. If they’ve already contracted with the vaccine maker, their contract is essentially holding their place in line — but they can, and should, offer that place to a country in more urgent need.
The US can certainly afford to do this. By July, Duke University researchers estimate, the country will likely have at least 300 million excess doses — and that estimate is assuming that the US will retain enough doses to vaccinate the vast majority of children. In other words, every eligible or soon-to-be-eligible American could get vaccinated, and there would still be 300 million doses left over — practically enough to give an extra dose to every person in the country.
A surplus of that magnitude is so staggering that not sharing it with the world starts to look morally unjustifiable.
What’s more, Aylward said countries shouldn’t focus only on donating excess doses. If they wait until they’ve vaccinated every eligible citizen, they’ll spend several more months immunizing people who are at relatively low risk, while adults at high risk in countries like India go unvaccinated. Instead, rich countries should act more like Sweden, which recently decided to donate 1 million of its doses — one-fifth of its current supply — even though just over 30 percent of its population has received a shot.
Do you have $7? If so, Covax wants your help.
This month, the WHO Foundation launched a fundraising campaign called “Go Give One,” which urges individuals to donate $7 to buy a vaccine dose for someone in a low-income country through Covax.
“There was huge popular demand among private individuals to contribute to address this important global issue, so this campaign gave an outlet to that demand,” a Gavi spokesperson said.
Faden said that if enough people were to contribute, it could potentially make a significant difference. “If you can come up with the money — say $7 — then of course you ought to do it,” she said. “At this point, it’s everyone’s responsibility. Everyone should be invested as a matter of obligation to global justice. Literally as a matter of duty.”
But she was clear that retail fundraising — getting small donations from many individuals — is not going to net Covax the billions of dollars it needs. That’s really a job for governments, and it requires the leaders of the world’s wealthy countries to step up.
Dodson personally donated to Go Give One and also ran a Facebook fundraiser for the campaign, which raised $1,000. “I feel really proud,” she told me. But she thinks the campaign’s main power may lie in its potential to catalyze government spending. “When governments see everyday individuals saying ‘We care about vaccine inequity, and we’re willing to put our pocketbooks against it,’ then that can help spur more political will.”
She also believes that advocacy in this arena is underfunded, though it can move the needle in a big way — as we saw when activist groups pressured Biden to back patent waivers. Arguably, donors could have a bigger impact by donating to an advocacy group than by donating to Go Give One, though this field is so new that it’s hard to know for sure.
For donors who prefer to invest in advocacy, Dodson and Glassman both recommended three groups: Global Citizen, the ONE Campaign, and the Pandemic Action Network.
“To the extent that advocacy movements help reduce the political cost of doing the right thing and create political benefits, I think it’s a good thing,” Glassman said. “And the amounts of money at stake that they could potentially influence are large, especially in the United States.”
Aylward, for his part, is hoping that more individuals and governments will start to show concern for the world by investing in Covax. “You’ve got this beautiful machine,” he said. “Put it to work.”